Study Shows ER Visits Up Under ACA







A study shows that ER visits have increased as more people have gotten coverage under the Affordable Care Act. This expected short term outcome isn’t ideal, but speaks to habits of the previously uninsured, the fact that ER visits are covered under the ACA, and an increased doc shortage as demand outpaces supply in the short term.
In the long term the healthcare provider workforce would be expected to grow and as people got used to having insurance more insured Americans would rely on primary doctors, urgent care, and other non-emergency solutions.

Emergency room visits may be up, but today more people are using insurance to pay for visits rather than simply sticking hospitals with unpaid bills.
Facts on Medicaid, ER Usage, and the New Report
We look at some facts behind the May 4th, 2015 American College of Emergency Physicians report on ER usage and the corresponding new 2015 acep poll affordable care act research results poll on ER usage below.
But first, let’s discuss the ER issue broadly:
- Before the ACA there was only one way for the uninsured to get healthcare, and that is the ER. This behavior hasn’t changed as more people get Medicaid coverage, despite efforts by HHS and other groups to spread awareness of how to use coverage.
- Under the ACA both Medicaid and Marketplace coverage cover emergency room visits as part of Ten Essential Benefits. That means all plans cover ER visits.
- The correct thing to do would be to make an appointment with a doctor in non-emergency situations, use urgent care in immediate but less drastic situations, and to only use the ER in true or perceived emergency situations like chest pain.
- The ACA incentivizes new doctors and healthcare workers, but adding healthcare providers to the workforce is something that happens over time. With uncertainty about the law and a spike in newly insured, demand is outpacing supply. Doctor wait times, especially for Medicaid and lower-premium Marketplace plans can be weeks or even months currently.
Facts from the American College of Emergency Physicians report on ER:
2,099 polls were completed with a 2.1% margin of error. About 60% worked for an emergency services company. 24% of member physicians polled practice in an emergency department with patient volume between 50,001-75,000, and 32% practice in emergency departments with patient volumes above 75,000.
- Most of the respondents to the poll report little or no reductions in the volume of emergency visits due to the availability of urgent care centers, retail clinics and telephone triage lines.
- About 90 percent of more than 2,000 respondents say the severity of illness or injury among emergency patients has either increased (44%) or remained the same (42%).
- More than one-quarter (28%) report significant increases in all emergency patients since the requirement to have health insurance took effect. In addition, more than half (56%) say the number of Medicaid patients is increasing.
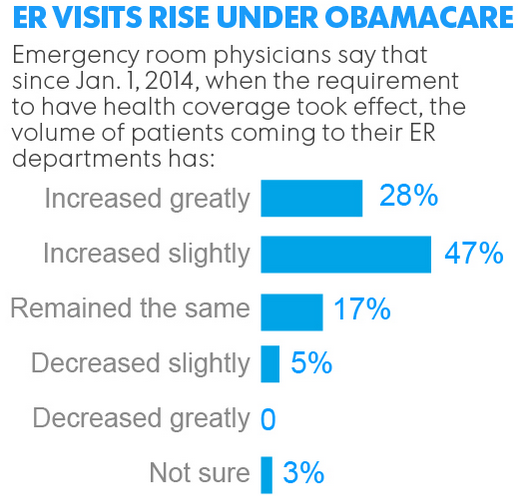
- Since the implementation of the ACA, the majority of member physicians have noticed an increase in the volume of emergency patients. Specifically, 47% of emergency physicians indicate slight increases in the number of patients, while 28% of respondents report significant increases in the number of emergency patients.
- Over half of emergency physicians indicate that the volume of Medicaid patients increased greatly (24%) or slightly (32%).
- 70% of member physicians believe their emergency department is not adequately prepared for potentially substantial increases in patient volume.
- Approximately 4 in 10 respondents report the acuity of emergency patients’ injuries or illnesses has remained the same since January 1, 2014. 44% of current members have noticed significant (14%) or slight (30%) increases in the acuity of emergency patients’ injuries or illnesses in their emergency department.
- Despite urgent care centers, 43% of member physicians report the volume of patients with less severe illness at their emergency department remains the same.
- For the majority of current members (49%), retail clinics have not changed the volume of patients with less severe illness at their emergency department. About one-quarter (26%) of respondents are unsure of the impact retail clinics have had on patient volume.
- 44% of respondents report that they are unsure how the volume of patients with less severe illness has changed. However, 39% of respondents indicate that the volume of patients with less severe illness remains the same.
- Notwithstanding the availability of more primary care options, the volume of patients with less severe illness remains relatively unchanged for 49% of respondents. 23% of current members are unsure about the impact of more primary care options on the number of patients.
- In spite of the reductions in reimbursement for emergency care, 66% of member physicians indicate that they have not considered leaving the practice of medicine, although 34% have considered leaving the profession.
- When asked if efforts are being made in their community or state to reduce the number of emergency patient visits, 41% of respondents report that no efforts are being made. 38% of respondents report that efforts are being made to decrease the number of emergency patient visits.
- Almost 6 in 10 current members’ communities or states are not actively involved in diverting Medicaid patients from the emergency department.
- 83% of member physicians have concerns about efforts being made to reduce emergency visits. Most respondents are concerned that patients will delay medical care or go to a less skilled site (44%). Other concerns about current efforts include their minimal impact on decreasing the volume of patients (44%) or lessening health care spending (41%).
- When asked how elimination of federal subsidies would affect emergency departments, 73% of respondents indicate that emergency visits will increase (42%) or remain the same (31%). Only 12% of current members report either that emergency visits will decrease (10%) or their emergency department will be at risk of closing (2%) if the government eliminated federal subsidies for health insurance.
- The majority of current members (65%) indicate that reimbursement for emergency care will decrease if the federal government were to eliminate federal subsidies for health insurance coverage in their state.
- 65% of respondents indicate that they have not stopped accepting payments from a health insurance plan or plans that are taking them out-of-network. Only 5% of current members have stopped accepting payment from a health insurance plan(s) that are taking them out-of-network.
- 64% of current members say that the time spent organizing patient care following visits to the emergency department has increased since January 1, 2014.
- 47% of member physicians believe demands for care coordination are increasing due to increased difficulty in finding/arranging timely follow-up with primary care physicians and/or specialists.
Heidy
I recently went to the ER and was admitted and told I needed surgery. During my stay, the doctor who performed the surgery was out or network and his assistant, who I’m told was not necessary for the procedure, is also out of network. I am now going through the process of appealing the decision made by my insurance of not paying for the procedure or assistant. Is there a law under the Affordable Care Act that can be of benefit for me?
ObamaCareFacts.comThe Author
The ACA expanded appeal rights, so if an appeal is denied it was part of what insured your right to appeal again.
Each time you appeal you may or may not be advised to escalate (for example from in-house appeal to external appeal).
Learn more: https://www.healthcare.gov/appeal-insurance-company-decision/appeals/
Lbinny
Obamacare was created to redistribute wealth and burden the working class who not only has to struggle to support themselves with higher deductibles that prevent them from getting the care they need but also make them responsible for people without insurance who can now get better care than themselves. The system has not addressed the real issues of poverty and cultural differences and most importantly individual accountability and responsibility. Obamas failed policies have been only beneficial for non-Americans and non- working people. Veterans and hardworking Americans have not benefited in anyway and feel that this administration has lied and deceived them. Activists that represent this Obama administration have divided our country and have made the lives of hardworking Americans decline and worse off during this time frame. Electing more democrats with unrealistic ideology will be be the ruin of our country.Healthcare along with any other change that Obama has instigated have failed miserably!
Jim H
You made a huge logical cause and effect leap without even a scintilla of empirical evidence. In your world poor apparently equals someone who for reasons you do not approve of do not work. Here’s a fact you ignored.
Of people eligible to work who are poor 63% work; however, the pay they earn is not enough to provide for themselves or their families. That fact alone tends to invalidate your cause and effect argument
Gerry Lisi
USA Today used these statistics to report that 3/4 of ED Physicians reported that ED visits “surged”. It seems to me that 3/4 of ED Physicians reported that ED visits increased slightly or were down to flat.
I can’t find publicly available ED visit data for my state for 2014. I’ll be anxious to see what the stats are.
ObamaCareFacts.comThe Author
According to the report on this page there wasn’t in fact much surging, but rather like you say a steady increase. The report isn’t saying unpaid emergency room visits are up (what happens when people don’t have insurance), but rather that emergency room visits are up in general. One would just assume more people covered = less reliance on emergency care and a bigger focus on primary care… but it looks like that is a behavior that has to be curbed over time. Certainly not economical to have non-emergency care done in the emergency room for America as a whole.
Robert Mazur
•’Before the ACA there was only one way for the uninsured to get healthcare, and that is the ER’. This is not true. In Savannah many patients can go to the Curtis Cooper Clinic, the JC Lewis clinic, and other for FREE clinics. These were in place long before the ACA. This has been true in other cities that I have worked in as well, such as SF, Seattle, Oakland..unfortunately, now patients with ‘insurance’ under the ACA, are not eligible for those centers, and therefore end up in the ER.
ObamaCareFacts.comThe Author
Valid point. This of course wasn’t an option for all uninsured people in all places, but it is certainly worth pointing out.
Chris
While the U.S. government continues to freely offer health care insurance subsidies (I believe most are substantial and relatively easy to qualify for), I wonder if it has ever given any thought to also subsidizing the education of nurses who wish to go into primary care as ARNP’s (Advanced Registered Nurse Practitioners). It appears that the shortage of primary care, and the difficulty in arranging it, is one of the factors that has led to increased ER usage since the advent of Obamacare. ARNP nurses are excellent deliverers of primary care and often do a better patient physical assessment than many physicians have ever even been taught to do.
ObamaCareFacts.comThe Author
The PPACA does a few things to incentivize the healthcare workforce, and nurses specifically. This includes, but isn’t limited to:
PPACA Title V – Subtitle D – Enhancing Health Care Workforce Education and Training
Go here and do a command find for “nurse” https://obamacarefacts.com/summary-of-provisions-patient-protection-and-affordable-care-act/